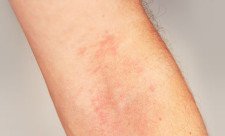
Our skin is colonised by vast numbers of bacteria, a normal condition even in the case of atopic eczema and other skin disorders. It is the makeup of this bacterial diversity that determines the health of our skin. The balance between healthy and less healthy bacteria also influences the skin barrier, i.e. the area that protects our skin from the intrusion of pathogen (= disease-causing) germs.
Researchers in Munich have looked into the correlation between the bacterial makeup of people suffering from atopic eczema and the effect of this makeup on the functioning of the skin barrier. More specifically, the scientists “wanted to find out what possible correlations exist between bacteria and those genes that maintain the skin barrier”, an article in the Ärztezeitung said. To this end, they collected skin samples from healthy subjects and from individuals with atopic eczema, according to information published by the Technical University of Munich.
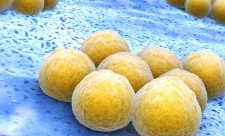
The result showed that the dominant bacterial species on the skin of atopic dermatitis patients are Staphylococcus aureus. In some inflamed skin samples, S. aureus actually accounted for up to 99 percent of the total microbial composition, said the report of the Technical University. In addition, S. aureus was also found to be particularly common on the skin of subjects which were affected, but did not yet show inflammation.
Conversely, this would mean that proactive application of skincare with microbiotic agents to stimulate the growth of healthy bacteria that confine S. aureus might delay the outbreak of the inflammations associated with the skin disorder.
What the scientists also found was that in inflamed skin, the activity of some genes was “significantly altered, depending on which bacterial inhabitants lived on the skin”. This means that such genes are involved in the maintenance of an intact and stable skin barrier – and conversely, that the balance of our skin flora might have an impact on our genes.
Dieser Post ist auch verfügbar auf: German

 28. Sep 2018
28. Sep 2018 Popular
Popular Recent
Recent Comments
Comments